The specialist I saw at my cardiopulmonary exercise testing (CPET; Keto: A New Approach To Reactive Hypoglycaemia) recommended establishing a sleep routine, which I only lost due to falling ill with a throat and chest infection that ended up lasting three months (Coronavirus, Self-Isolation, And The Selfishness Of Others). Now the specialist from the Department of Psychological Medicine was saying the same, but this time they wrote a prescription for a medication to help me sleep. That medication was melatonin.
Some Background Information
I got a referral to attend the Department of Psychological Medicine and Integrated Care, and the doctor who prescribed the melatonin medication worked in this department. The department itself was created to give a holistic approach to treatment by combining mental and physical healthcare. Which is certainly a good concept for a department.
Before I was put on the beta-blockers at a dose that worked for me, my heart condition and my anxiety used to cause a negative feedback loop for each other. My anxiety would worsen palpitations and chest pains, and vice versa. And I now know that my hypos can also trigger my anxiety due to feelings of muscle weakness and risk of passing out.
The prescribing doctor told me that melatonin was a natural hormone, and the medication was pitched to me as basically being a natural hormone. The doctor also told me that I’d be able to take this sleeping medication for as long as I needed to, because it’s not an addictive drug, and because it’s just a natural hormone.
The natural hormone, melatonin, is produced by the pineal gland, which is located in your brain (NHS). This hormone helps regulate your sleep/wake cycle (Wikipedia).
However, the doctor who prescribed the melatonin medication denied there were any side effects of taking this medication, they were wrong. There are always possible side effects of taking any medication, even melatonin.
The NHS website listed the following side effects:
Common side (1 in 100 people)
- Feeling sleepy or tired in the daytime.
- Headache.
- Stomach ache or feeling sick (nausea).
- Feeling dizzy.
- Feeling irritable or restless.
- Dry mouth.
- Dry or itchy skin.
- Pains in your arms or legs.
- Strange dreams or night sweats.
Serious side effects (1 in 1000 people)
- Start feeling low or sad – this could be a sign of depression.
- Get blurry vision or your eyes become more watery than usual.
- Feel faint or pass out.
- Start feeling confused or dizzy, or things seem to be spinning around you (vertigo) – Not ideal for someone like me with Persistent Postural-Perceptual Dizziness (PPPD).
- Have any bleeding that does not stop, unexplained bruising or blood in your urine.
- Get psoriasis.
However, I didn’t get any of these side effects; I got something far more worrying.
Medication Interaction
I took the first tablet as instructed and it caused my eyes to feel heavy and I felt really tired for the first 30 minutes. However, that wasn’t all that happened.
I started getting chest pains within 30 minutes of taking my first melatonin tablet. This lasted almost three hours. The same happened for the next three nights when I took it, so I decided to stop taking it. However, five days later, I still had chest pains, and for about eight hours on the fourth day, I had palpitations as well. Not good.
I was unable to sleep as these chest pains stayed with me for a solid six hours. I also became concerned about what would happen if I went to sleep with these incredibly debilitating chest pains. I talked to my partner about it and convinced me to try the medication the following night, but this time I didn’t even get the heavy eyes and tiredness, I just got chest pains.
It took seven days before the chest pains stopped being constant, but I was still getting them occasionally for a full month later. That’s a long recovery time from this medication before everything returned to normal, my normal at least.
These symptoms were either an unreported side effect of taking the melatonin, an issue specific to my heart condition and that medication that was unknown, or a negative interaction between the melatonin medication and the beta-blockers I take for my heart problem.
The prescribing doctor of the melatonin medication had told me that beta-blockers can affect natural melatonin levels, which could be why I’m struggling to sleep.
This does appear to be true. According to a study by Stoschitzky et al. (1999), who performed a small double-blinded, randomised, placebo-controlled, cross-over study with 15 participants, beta-blockers reduce melatonin release via specific inhibition of adrenergic beta1-receptors.

So if beta-blockers really do reduce the body’s melatonin production, then is it possible that raising it again with melatonin medication could cause the beta-blocker to stop working as it should do? This is my hypothesis.
However, before I formed this hypothesis, I did first consider if it was possible that these chest pains and palpitations were somehow psychosomatic.
This isn’t the first time I’ve had to consider if some of my issues were psychosomatic. However, each time I’ve considered this, it’s always turned out not to be the case, and this time was no different.
My anxiety disorders have never caused palpitations or chest pains before because whenever my anxiety rises high enough for my body to produce adrenaline, I would have a psychotic episode instead.
Furthermore, by the time I developed my autonomic disorder that causes my heart palpitations, I’d already worked on myself to massively reduce my psychotic episodes. This meant my anxiety wasn’t triggering any releases of adrenaline anymore, so there could be no way my anxiety was causing my heart problems. There is more than a three-year gap between the two. Thus, it’s very unlikely that my mental health is a causal factor in my heart problems.
I’ve also taken sleeping pills before (I’ve suffered from Insomnia before for years), more than three different types, over a number of years, and I didn’t have any side effects from them. So it seems improbable that the melatonin causing the chest pains and palpitations would be psychosomatic instead.
However, all my prescribing doctors cared about is blaming it on my anxiety, even though my anxiety doesn’t cause chest pains or palpitations, and hasn’t come close to causing either in over three years. Plus, since starting on my beta-blockers, I rarely have any palpitations or chest pains, and that’s been about seven years now. So it’s clearly not my anxiety. The only new variable in my life is the melatonin medication.
Reporting Medication
I decided to report what happened as a side effect/unforeseen interaction with my beta-blockers, to help make sure this medication is used and prescribed safely. I wouldn’t want someone else to have the same reaction as me, or worse.
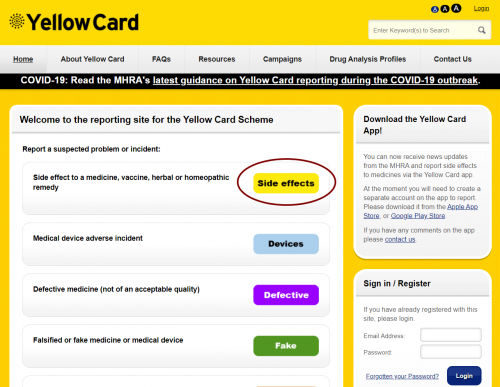
Should you ever find yourself having similar issues with medication or an issue with medical equipment, you can do so using the following link if you live in the UK: Yellow Card.
This will be the first medication I’ve ever made a report for, as the times my antidepressants caused me to have psychotic episodes I felt was unique to me (Taking Antidepressants And Being Forced To Go Cold Turkey), because everything that affected my homeostatic system triggered it, from over-the-counter painkillers to Redbull.
Before I could fill in the form, I realised there wasn’t a headline that directly applied to what I was trying to report: An interaction between two medications. So I emailed them for clarity. They replied, stating that ‘Side Effects’ was the correct option to select, as the suspected medications would be assessed with consideration of their effects both in isolation and in combination.
As always, leave your feedback in the comments section below. Also, feel free to share your experiences with medication side effects and strange interactions in the comments section below as well. If you want to stay up-to-date with my blog, then sign up for my newsletter below. Alternatively, get push notifications for new articles by clicking the red bell icon in the bottom right corner.
Lastly, if you’d like to support my blog, then you can make a donation of any size below as well. Until next time, Unwanted Life readers.
References
Stoschitzky, K., Sakotnik, A., Lercher, P., Zweiker, R., Maier, R., Liebmann, P., & Lindner, W. (1999). Influence of beta-blockers on melatonin release. European Journal of Clinical Pharmacology, 55, 111–115. Retrieved from https://doi.org/10.1007/s002280050604.

I didn’t know you could report medication like that, thanks for that information. I’m amazed a doctor tried to claim had no side effects, like you said everything does.
You’d think they’d make something as important as reporting medication a lot better known than they currently do
Good post. I learn a lot of things about mental health by reading your blog. I pray that your life will get better. You are a good person. You must believe that.
The advice in this post also relates to those taking medications for their mental health, as they can also cause problematic interactions and side effects as well
I”m so sorry for the experience you went through – that sounds terrible! Good for you for reporting the side effects to them so others do fall victim to the same reaction! Or at least have warning of the possibility!
I’d hate to think what would have happened if that reaction happened to someone older with poorer health than me
What a scary, long lasting side affect! I hope you are feeling better now and on the road to getting better sleep.
My sleep is still screwed up, but I’d rather that then my heart problems being like they were
These interactions are dangerous. Unfortunately, Doctors are ordinary people
Drug interactions are indeed dangerous, which is why I was so concerned about what happened to me, leading me to reporting it
Thank you for this post! It is very important to keep well-informed! 🙂
Indeed it is
I am so sorry for what you went through; I had chest pain from anxiety attacks once but this sounds a dozen times worse! I love that you made a clear report, though, so that the medication can be used more safely in the future, and I hope you can find a good medication that works for you in as healthy a way as possible. 🙂
Sorry to hear about your experience with chest pains, I hope that’s no longer an issues for you
Happily, it cleared up fairly quickly! I hope you find a solution too. 🙂
I think my heart issues is a life long issue now, but as long as my medication works, it’s not a problem
Wow, I’m so sorry you had a bad reaction. You know your body best, and it’s always a good idea to learn about potential side effects of drugs and supplements. It is possible to be allergic to anything, too.
Good point, I hadn’t considered allergic reactions
Vitamins and herbs are too poorly regulated, so it’s good that you spoke up! And are raising awareness here, too.
http://www.susanberkkoch.com/blog
They are indeed poorly related, but you can also report those that claim to be medication too
I think it’s great you take the time to gather the info.
Thanks
Whoa, that is a bad reaction. I hope things get better soon with these medications
Thank you
Thank you for sharing! Very informative. What an awful experience you went through.
Thanks for reading
This is an awesome post. I think you are helping a lot of people right now who didn’t know some of this stuff.
It would be nice if it helped someone ?
Wow, I’m so sorry you had a bad reaction. It’s great that you are sharing your experience here so others can learn from it. I think it’s scary sometimes how much blind trust we put in our doctors. They are human too after all. And humans make mistakes. Thanks for sharing.
It’s not just doctors we put a lot of blind faith in, which can often lead to other more dangerous problems
This makes so much sense! I take a beta-blocker for my migraines and last month my medication stopped working, during those weeks I was taking a supplement that contained melatonin. I just realized I haven’t gotten a migraine since I stopped taking that supplement. The really should label that.
At least there’s some good news about being migraine free since stopping the supplement
It’s good to see that they have made it so easy to report issues like this. I would think the ease of use of Yellow Card would encourage people to report things that they may have otherwise let slide due to the hoops that they would have to jump.
I’d certainly let such things slide before simply because I had no idea the Yellow Card system existed before this recent medication interaction
As a health care provider, I’m sorry to hear you went through this! Glad things are much better
Thanks