I was first inspired to write this article after my long, long, long struggle to get support for my eating disorder. Being a big Black guy, my issues were constantly being ignored and dismissed. However, the idea for this article just sat in my rough draft ideas for ages. That is, until I saw the theme of America’s Black History Month, Black health and wellness, which you can find more information on by clicking here.
Thus, I thought now might be a good time to write and publish my article on Black health and wellness and its links to racism in medicine. I know, it’s not quite on the theme of Black History Month, but it’s something that needs to be talked about.
Black Health And Wellness: Black Women And The Pregnancy Disparity
I recently came across an article by Huffington Post that also helped rekindle my desire to cover this topic as a Black man. That’s because whenever you look at posters or information on health conditions, they always feature photos and illustrations of White people, and that’s a problem.
The problem isn’t just about representation, it’s also dangerous. People have died because medical professionals don’t know how to recognise symptoms in people with dark skin. For example, babies with jaundice have a yellow colouring of the skin and eyes, but if you have dark skin, it’ll be very hard to notice yellowing of the skin as a symptom (KidsHealth). And that’s only the start of the problems the Whitewashing of medical training and health textbooks cause.
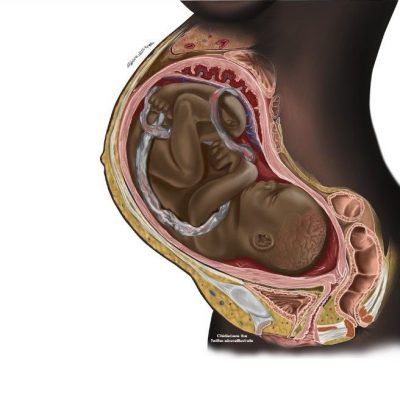
Chidiebere Sunday Ibe from Ebonyi State, Nigeria, wanted to do something about that and began illustrating Black patients, children, and babies. One such image, a drawing of a Black foetus and mother, went viral on Twitter and TikTok. You can see that image below.
United Kingdom
Black Ballad, a lifestyle publication, conducted a survey on motherhood about Black British women in 2020 that got 2,500 participants. The results showed that Black British mothers are five times more likely to die in childbirth due to pregnancy complications than their White counterparts. The survey also highlighted that Black British mothers would experience substandard care, discrimination, wrong doses of medication, and abuse that put their pregnancies at risk (Huffington Post).
This shocking finding supports the existing findings by Knight et al. (2019), who reported that there remains a five-fold difference in maternal mortality rates amongst women from Black ethnic backgrounds compared to White women. But it doesn’t stop there. They also found a three-fold difference in women of mixed ethnicity and an almost two-fold difference among women from Asian ethnic backgrounds when compared to White women.
To see two ITV News stories that discuss this problem, click here.
Click here to watch Channel 4’s Dispatches documentary: The Black Maternity Scandal.
United States of America
Although the UK has a long way to go with maternity care for Black women, the US isn’t doing much better. According to the Centers for Disease Control and Prevention (CDC), Black women are three times more likely to die from a pregnancy-related cause than their White counterparts are. The CDC lists several factors involved in this, with structural racism and implicit bias being the ones that speak louder.
It should be noted that this appears to be an improvement on America’s previous figures for Black women and pregnancy-related deaths when compared to their White counterparts. Previously, the figure was between 2-6 times more likely to die, with certain states doing worse than others (CDC, 1999). Here’s looking at you, Texas.
To read Serena Williams’s scary childbirth story, click here.
Lancet report
The issues for Black women and pregnancy don’t just happen during giving birth and the year post childbirth. The Lancet analysed the data of 4.6 million pregnancies across seven countries and found that the risk of miscarriage for Black women is 43% higher than their White counterparts (BBC). However, the risk of miscarriage could be reduced if medical professionals were trained to understand the health of Black and other ethnic groups, rather than being taught only about it from a White perspective.

Black Health And Wellness: Medication And Pain
There’s a long history of giving the wrong doses of medication to Black people that is rooted in racism, rather than anything medical. It’s the same implicit bias that kills pregnant Black women that rears its ugly head again with medications.
There is a myth that Black people don’t feel pain as much as their White counterparts do. Meaning, throughout history, Black people, especially Black women in childbirth, were not given enough pain medication or weren’t given any. Because of implicit bias, Black people still aren’t being listened to (Today).
One of the most horrifying examples of this ridiculous belief comes from James Marion Sims, the so-called ‘Father of Modern Gynaecology’. Because of this ludicrous belief around pain, this physician conducted medical research on enslaved Black women without anaesthesia.
A study by Hoffman, Trawalter, Axt, and Oliver (2016) confirmed the Black pain myth in America. They also found that first, second, and third-year medical student participants who believed this myth made less accurate treatment recommendations. Which is a worrying finding for the safety of Black people seeking medical care.
To add insult to injury, according to Singhal, Tien, and Hsia (2016), there is also a significant racial-ethnic disparity in opioid prescription and administration in US emergency departments. Black people are half as likely to be prescribed opioid medicines. The reason is that the unconscious biases these medical professionals have meant they think Black people are more likely to fake pain to feed their substance dependency.
The reality is, that the rates of “illicit” drug use aren’t significantly different between Blacks and their White counterparts (Meghani, Byun, and Gallagher, 2012), but they’re treated as if there is.
Other Black Health And Wellness Myths That Still Exist
Lindsay Tweeted an image from a book called ‘Nursing: A Concept-Based Approach to Learning’ which contained some unbelievably outdated views about other ethnic groups. The book in question was published in 2017!
this page is from a medical textbook that was published in wait for it…2017. pic.twitter.com/R5DV7ZqxJM
— lindsay (@lindsaaaytweets) July 1, 2020
Another finding from Hoffman, Trawalter, Axt, and Oliver (2016) study was that about 50% of their medical student participants reported that at least one of the false belief items listed in the study was probable or definitely true. To give that context, these beliefs were stuff like: Black people’s skin is thicker than White people’s skin, Black people age more slowly than White people and even White people have larger brains than Black people.
As stated at the start of the article, people Black people’s health issues aren’t always as obvious as their White counterparts, as with other ethnic groups. When you add this to the Black myths medical professionals can have, it creates a two-tier healthcare system.
Implementing Change
Implicit bias in healthcare professionals is a well-established fact, and the root cause of most issues when it comes to Black Health and Wellness (FitzGerald and Hurst, 2017). Thus, the first step we all need to take is to train all medical professionals about implicit bias. A key part of this is teaching children, teens, and young adults about not only the biases we all have but about racial inequality as well, such as teaching critical race theory in the US. Awareness is the key to overcoming such problems.
We need to move away from the longstanding medical concept that the White male model is the default for all of us. This will not only save the lives and Black people and other ethnic groups but also White women. That’s because the doses required for medication can be different between the sexes.
Furthermore, until the above changes can bear fruit, we need to take steps to help us now. For example, we need to create clinical guidelines, standardised checklists, and system-wide protocols that remove medical professionals from deciding based on their implicit bias to avoid it affecting patient care (AAMC).
Another option is to keep abortions safe and legal, which can save countless lives that might be lost to pregnancy complications. Stevenson‘s (2021) research found that banning abortion in America would lead to a 21% increase in the number of pregnancy-related deaths for all women, but a 33% increase among Black women, compared with rates for 2017.
We need to remember that even though pain is subjective, which is why patients are asked to rate their pain on a scale, this subjective nature isn’t rooted in our ethnic backgrounds. It’s because of individual differences.
Summary
In this day and age, it boggles the mind that health professionals still have the same kinds of outdated views of Black people’s biology as they did during the slave trade. But unfortunately, that’s still our reality as the world continues to deal with its long-ingrained institutional racism.
The wider implications of Black health and wellness and the Black myths that still exist don’t just stop with Black people. These can affect anyone who isn’t White. If medical professionals are only trained to recognise symptoms in White people, then anyone with skin that isn’t white could find their health at risk.
We can do better, and we will do better. All that’s needed is for policies and changes to be implemented and we’ll all be better off for it. Because a medical field that conducts its research on participants who aren’t just White men, and trains our medical professionals accordingly, will create a workforce who instinctively knows that illnesses can present in many ways. Rather than having a medical field that only looks for the typical ways they present in White people, as we still do today.
As always, leave your feedback in the comments section below. Also, please share your experiences with Black health, wellness myths, or general racism in medicine in the comments section below as well. Don’t forget, if you want to stay up-to-date with my blog, then sign up for my newsletter below. Alternatively, get push notifications for new articles by clicking the red bell icon in the bottom right corner.
Lastly, if you’d like to support my blog, you can make a donation of any size below. Until next time, Unwanted Life readers.
References
Centers for Disease Control and Prevention (CDC). (1999). State-Specific Maternal Mortality Among Black and White Women–United States, 1987-1996. MMWR. Morbidity and mortality weekly report, 48(23), 492-496. Retrieved from https://jamanetwork.com/journals/jama/fullarticle/1842508 and https://www.cdc.gov/mmwr/preview/mmwrhtml/mm4823a3.htm.
FitzGerald, C., & Hurst, S. (2017). Implicit bias in healthcare professionals: a systematic review. BMC medical ethics, 18(1), 1-18. Retrieved from https://bmcmedethics.biomedcentral.com/articles/10.1186/s12910-017-0179-8 and https://doi.org/10.1186/s12910-017-0179-8.
Hoffman, K. M., Trawalter, S., Axt, J. R., & Oliver, M. N. (2016). Racial bias in pain assessment and treatment recommendations, and false beliefs about biological differences between blacks and whites. Proceedings of the National Academy of Sciences, 113(16), 4296-4301. Retrieved from https://www.pnas.org/content/113/16/4296.full, https://www.pnas.org/content/pnas/113/16/4296.full.pdf, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4843483, and https://doi.org/10.1073/pnas.1516047113.
Knight, M., Bunch, K., Tuffnell, D., Shakespeare, Kotnis, R., Kenyon, S., J., & Kurinczuk, J. J. (Eds.) on behalf of MBRRACE-UK. (2019). Saving Lives, Improving Mothers’ Care: Lessons learned to inform maternity care from the UK and Ireland Confidential Enquiries into Maternal Deaths and Morbidity 2015-17. Oxford: National Perinatal Epidemiology Unit, University of Oxford. Retrieved from https://www.npeu.ox.ac.uk/assets/downloads/mbrrace-uk/reports/MBRRACE-UK%20Maternal%20Report%202019%20-%20WEB%20VERSION.pdf.
Meghani, S. H., Byun, E., & Gallagher, R. M. (2012). Time to take stock: a meta-analysis and systematic review of analgesic treatment disparities for pain in the United States. Pain Medicine, 13(2), 150-174. Retrieved from https://academic.oup.com/painmedicine/article/13/2/150/1935962 and https://doi.org/10.1111/j.1526-4637.2011.01310.x.
Singhal, A., Tien, Y. Y., & Hsia, R. Y. (2016). Racial-Ethnic Disparities in Opioid Prescriptions at Emergency Department Visits for Conditions Commonly Associated with Prescription Drug Abuse. PloS one, 11(8), e0159224. Retrieved from https://doi.org/10.1371/journal.pone.0159224, https://pubmed.ncbi.nlm.nih.gov/27501459, and https://dx.plos.org/10.1371/journal.pone.0159224.
Stevenson, A. J. (2021). The Pregnancy-Related Mortality Impact of a Total Abortion Ban in the United States: A Research Note on Increased Deaths Due to Remaining Pregnant. Demography, 58(6), 2019-2028. Retrieved from https://read.dukeupress.edu/demography/article/58/6/2019/265968/The-Pregnancy-Related-Mortality-Impact-of-a-Total and https://doi.org/10.1215/00703370-9585908.


This is interesting and alarming at the same time. Thanks for sharing.
Thank you
This was a very informative & interesting read. I agree that there is a racial bias in the medical field. A lot of it does stem from lack of information. But we must keep talking about it and creating new source material and pushing aside the preconceived biases and stereotypes that have defined many races & ethnic groups for so long.
It’s a conversation that has to be kept in the public eye if we’re ever going to get the changes we need to have safe healthcare for all
Thank you so much for sharing this interesting and illuminating piece. I am so sorry you faced this issue- and I think it’s important you’re raising awareness of this issue
At least my run ins with it haven’t cost me my life, yet
Not sure why the like button isn’t loading but thank you for writing such a detailed article! The racism and or bias in medicine really needs to end as it is putting lives at risk. I’m hoping as more awareness is raised the field will make the required changes.
It certainly would be nice if we could put the issue to bed once and for all
Thanks for this informative post. It’s shocking to me that this kind of bias still exists in our world—but even moreso among educated, intelligent people. It’s a sad statement about how behind the times some of our “advanced” educational institutions are. Academia moves slowly in many ways.
Indeed it can move far too slowly
Very informative article. It’s awful that racism and biased views prevent non white people from getting the health care they need
It’s shocking that these issues still exist
Wow, the studies are shocking and thank you for highlighting this as it can help others as well.
They really are shocking
I am horrified by these facts and statistics. Thank you for shining light on an important and clearly unspoken topic.
Yeah, a lot still needs to be done to remedy this problem
This is so important to keep talking about it…
So important
I’m genuinely shocked and horrified and hope things change very soon.
So do I
Thank you for this post! It’s super important to spread awareness about this. Praying things change soon as they should long time ago…
If only praying was enough to make things happen
This is the perfect type of post for Black History Month! Increasing awareness of systemic racism and implicit bias in the medical setting is important at any time. It seems almost impossible to avoid repeating history in one way or another, but hopefully efforts to raise cultural competency will contribute to positive change.
We do seem to be creatures of habit when it comes to not learning from the past. But hopefully we’ll be able to break that cycle for good one day
As a black woman and the mother of a black daughter, this hit so close to home. I talk about it all the time because it’s just so infuriating. I challenge people of all races to “Google” a common childhood issue, such as “rash 4 year old” or something similar. When looking at images, unless race is specified in the query, the images are all of white children. It may surprise people to know that parents of kids in all shades want to see how something might look on their child. I read something in my colleges newsletter that said the test for kidney disease (i believe) looks different for black people than it does white people, but that the prognosis and treatment doesn’t acknowledge that.
The issue is that the medical knowledge being shared is, as you noted, inaccurate. I would like to believe that as diversity increases in the medical field, knowledge will as well, but that’s not the case. Those doctors/ nurses are still learning from the same books. I could go on and on because this just makes me crazy. I planned on blogging about this as well and may still in the future. Thank you for taking the time to share this disparity that is, quite literally, killing people.
~ Cassie | letsgrowmom.com
I hope you do still blog about this, the more people we get talking about this the closer we get to making the changes that are needed
Thank you so much for sharing such a educational and interesting blogpost. I had no idea how bad things were in the medical field and I’m so sorry you’ve faced what you have. Hopefully change will begin to happen. Xo
Elle – ellegracedeveson.com
Hopefully that change will be swift and far reaching
Such an important topic to write about it. This has been an issue in the medical field for far too long. Although I am not Black, I am a minority and I remember the state of panic I had going into labor because I felt the doctors would not take the best care of me. I heard horror stories from other women and how medical professionals do not take the time to listen to their patient’s concerns, or even take what the patient is saying seriously. My daughter is half African and just to get a proper diagnosis of eczema was difficult because as opposed to have red, patchy skin, her skin became discolored in certain areas. Thank you for shedding light on this topic and sharing your experience.
Thank you for sharing and providing us with another example of how a condition can present differently in people with darker skin
I knew racism in the medical field was an issue, but I didn’t realize the extent such as black women being 3-5 times more likely to die during childbirth and black people not being given any or enough pain medication. Thank you for talking an important topic and I hope that changes will happen soon.
I hope the changes happen soon too
Yes, you’re right. I do still need to write about it. Thanks again for sharing your perspective.
I look forward to reading your piece
This was very insightful, thank you. I appreciate all the emotional labour that went into this!
Thanks for reading
This is such an eye-opening and insightful post. Thank you for sharing this!
Thanks for reading
You’re welcome.
Racial Health Disparity among African Americans in the medical field is so prevalent here in the US; it is so easily swept under the carpet. I have experienced it so many times.
As African Americans, if we are not our own health advocate, we can end up “6 foot 6.” More people, especially celebrities, should use their platforms to shed more light on this growing issue. Thanks for your contribution. Side note: had no idea you were a African American Brother.
I’m not African American, I’m British born and bred, but I am black ✊?
Thank you for sharing. Very informative.
??
Speaking truth to power. Continue to do it as eloquently as you do.
I’ll try ✊?
I cannot BELIEVE that textbook excerpt is from 2017! That it even has such a section is bad enough, but the contents take it to a whole other level.
Loved the educational value of this post in conjunction with the evidence and stories you share. It is important to keep passing the torch along and keep the light shining in the ignored corners. 🙂
It’s really disturbing how some textbooks are still being made
I learn so much from reading your blog. Keep up the hard work.
Thanks