Not too long ago, I watched a BBC documentary called: Daisy Maskell: Insomnia And Me. I’ve struggled with insomnia pretty much all my life, so I was really interested in watching this BBC Three show. And I’m glad I did. I learnt of a new CBT technique that’s designed to help people with insomnia, CBT-I, so I’m sharing it with you.
What Is CBT-I?
First, for those who are unaware of what insomnia is, which probably means you don’t have sleep issues (lucky), insomnia is a common sleep disorder which makes it difficult to fall asleep, difficult to stay asleep, and causes you to wake up early. In short, you never get enough hours of good quality sleep. According to Koffel, Bramoweth, and Ulmer (2018), insomnia affects nearly a quarter of the US population, with at least a third being affected in the UK (Swift, Stewart, Andiappan, Smith, Espie, and Brown, 2012).
Oh, I should also tell you what CBT-I stands for, just in case. CBT-I stands for Cognitive Behavioral Therapy for Insomnia. Pretty straightforward. CBT-I explores the connection between how we think, the things we do, and how we sleep (Sleep Foundation).
CBT-I claims to be an effective treatment for insomnia, which uses a structured programme to identify and replace behaviours and thoughts that worsen your sleep issues with new habits to improve your sleep quality (Mayo Clinic).
How Can CBT-I Help Me Sleep?
An alternative to medication
This tops my list because taking sleeping pills isn’t a long-term solution. Sleeping pills can be addictive, and even if you don’t become addicted to them, no ethical doctor will prescribe them forever. Plus, there are side effects to factor in and long-term costs, if you don’t have universal health care like my American readers. Thus, CBT-I could solve your sleep problems without having to take medication.
Tackles the root cause
CBT-I helps you identify and overcome the root cause of your insomnia. There are a lot of other health and mental health conditions that have sleep issues as a symptom. For example, depression has sleep disturbance as a symptom. Thus, you may not realise you’re depressed and just think you have a sleep problem, but a course of CBT-I might identify the true cause as being depression. You can then get appropriate treatment to tackle the underlying cause of the depression.
Insomnia is a co-occurring condition with a lot of mental health disorders (Taylor and Pruiksma, 2014). As such, getting to the root cause of your insomnia is important.
Online
Because of how beneficial CBT-I is with treating insomnia, there is a push to create online CBT-I platforms and apps. You could skip seeing a therapist and use CBT-I as a self-help technique instead, so don’t be afraid to Google for online CBT-I options so you don’t have to wait to get support from a therapist.
Fortunately, Erten Uyumaz, Feijs, and Hu (2021) have reviewed several readily available CBT-I apps that you can download to help with your insomnia. All were reviewed based on their CBT-I merits and usefulness (see below).
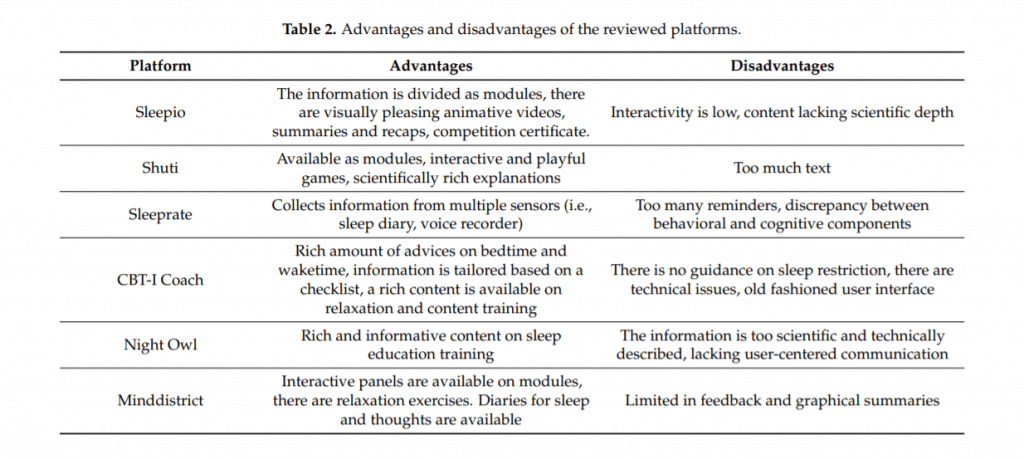
Techniques
Sleep diary
A sleep diary is a pretty basic technique but one that can help identify the issues that need working on. Keeping a diary of your sleep habits will help identify patterns, which can lead to solutions. There’s even an app that could help with tracking this information, which I recently reviewed, and that’s the Bearable app. Click here to read the review.
Stimulus control
This is a combination of tackling the worry and frustrations you have that affect your ability to sleep while also removing barriers that have conditioned your mind to resist sleep.
Sleep rescheduling
Here you’ll look at fixing your sleep schedule by identifying the best time to go to bed and wake up so you can establish a new sleep pattern.
Sleep restriction
This one may sound counterproductive, but it’s not. I don’t know about you, but if I try to go to sleep before I’m tired, I end up having less sleep or almost no sleep at all. Therefore, this method stops you from trying to force yourself to sleep by disregarding laying in bed if you’re not tired. You might use this method if the sleep rescheduling isn’t effective, in which case you’ll return to sleep rescheduling once your sleep quality improves.
Sleep hygiene
With this technique, you’ll be discussing lifestyle changes that can be made to improve your quality of sleep. This could mean tackling your smoking, as nicotine is a stimulant, as is caffeine. Therefore, you might have to stop using either stimulant after a certain time, cut back on their use, or even think about going abstinent.
It could also mean cutting down on alcohol because alcohol stops you from getting a good night’s sleep. That’s why you often wake up still feeling extremely tired after a session the night before with your mates. Drinking alcohol to help you sleep simply doesn’t work, because you can’t get the type of sleep your body needs.
You’ll also talk about setting up a sleep routine to help you wind down at night. Having such a routine will help train your body to prepare to go to sleep. And, this one might not be so popular, but exercising will be something you might have to do to help make your body feel tired.
Putting the day behind you
Pretty self-explanatory. It simply means you need to clear your mind of what happened during the day by working through them before trying to sleep.
Distraction techniques
If trying to put your day to rest doesn’t help before trying to sleep, or if you’re like me, your mind will always find something to fill the silence, then you’ll be taught some distraction techniques to use. For me, sleeping with the TV on helped, but that goes against the following technique.

Sleeping environment
Basically, you’re meant to make your bedroom a bedroom. You can do this by keeping it quiet (telling you sleeping with the TV on goes against this technique), making the room dark, keeping the bedroom cool, hiding the clock, don’t have a TV in there, etc. Just not possible for me. I live in a single room that is my bedroom, my living room, and my dining room. Not an ideal living situation during the pandemic, either. Having another room to exist in would have been nice these last 20 odd months.
Relaxation
This could be simply teaching you relaxation methods to use before bed, but also ways to manage stress and even anxiety. You’ll learn many ways to quiet your body and mind, such as meditation and breathing exercises.
Paradoxical intention
Instead of trying to make yourself sleep, this method will seek to do the opposite. You’ll try doing nothing to help yourself sleep because, for some, the effort of trying could make it harder for them to sleep. In short, you’ll be trying to learn to let go of the worry around your insomnia. If you sleep, great, if you don’t, it doesn’t matter.
Review and relapse prevention
If you’re getting good CBT-I, then you’ll also review your progress and be taught how to avoid relapsing into old sleeping habits and how to reestablish healthier sleeping habits should you have a lapse.
How Effective Is CBT-I?
A study by Taylor and Pruiksma (2014) reviewed previous studies into insomnia and co-occurring mental health conditions (depression, PTSD, substance dependency, and anxiety), finding that CBT-I was effective in treating insomnia and often helped the co-occurring disorder too.
Support for this comes from Swift, Stewart, Andiappan, Smith, Espie, and Brown’s (2012) day-long community CBT-I programme study, finding it to be effective in treating insomnia. Further support for CBT-I effectiveness comes from Waters, Chiu, Dragovic, and Ree (2020) who found it also works with people who have psychosis, like me.
And, just to round out this section with one last bit of supporting information, Fleming and MacMahon (2015) outline how many clinical trials have established the effectiveness of CBT-I in the general population and, more recently, in those who have insomnia as a consequence of having cancer. This caught my eye because my mum had cancer, my nana died of cancer, and my uncle has had cancer twice.
As always, leave your feedback in the comments section below. Also, feel free to share your experiences with CBT-I and insomnia in the comments section below as well. Don’t forget to bookmark my site and if you want to stay up-to-date with my blog, then sign up for my newsletter below. Alternatively, get push notifications for new articles by clicking the red bell icon in the bottom right corner.
Lastly, if you’d like to support my blog, you can make a donation of any size below. Until next time, Unwanted Life readers.
References
Fleming, L., & MacMahon, K. (2015). CBT-I in cancer: we know it works, so why are we waiting?. Current Sleep Medicine Reports, 1(3), 177-183. Retrieved from https://doi.org/10.1007/s40675-015-0021-0 and https://link.springer.com/article/10.1007/s40675-015-0021-0.
Erten Uyumaz, B., Feijs, L., & Hu, J. (2021). A review of digital cognitive behavioral therapy for insomnia (CBT-I apps): are they designed for engagement?. International journal of environmental research and public health, 18(6), 2929. Retrieved from https://doi.org/10.3390/ijerph18062929 and https://www.mdpi.com/1660-4601/18/6/2929.
Koffel, E., Bramoweth, A. D., & Ulmer, C. S. (2018). Increasing access to and utilization of cognitive behavioral therapy for insomnia (CBT-I): a narrative review. Journal of General Internal Medicine, 33(6), 955-962. Retrieved from https://doi.org/10.1007/s11606-018-4390-1 and https://link.springer.com/article/10.1007/s11606-018-4390-1.
Swift, N., Stewart, R., Andiappan, M., Smith, A., Espie, C. A., & Brown, J. S. (2012). The effectiveness of community day‐long CBT‐I workshops for participants with insomnia symptoms: a randomised controlled trial. Journal of Sleep Research, 21(3), 270-280. Retrieved from https://doi.org/10.1111/j.1365-2869.2011.00940.x, https://onlinelibrary.wiley.com/doi/pdfdirect/10.1111/j.1365-2869.2011.00940.x, and https://onlinelibrary.wiley.com/doi/full/10.1111/j.1365-2869.2011.00940.x.
Taylor, D. J., & Pruiksma, K. E. (2014). Cognitive and behavioural therapy for insomnia (CBT-I) in psychiatric populations: a systematic review. International review of psychiatry, 26(2), 205-213. Retrieved from https://doi.org/10.3109/09540261.2014.902808 and https://www.researchgate.net/profile/Daniel-Taylor-23/publication/262811349_Cognitive_and_behavioural_therapy_for_insomnia_CBT-I_in_psychiatric_populations_A_systematic_review/links/55ca2ea908aebc967dfbdd21/Cognitive-and-behavioural-therapy-for-insomnia-CBT-I-in-psychiatric-populations-A-systematic-review.pdf.
Waters, F., Chiu, V. W., Dragovic, M., & Ree, M. (2020). Different patterns of treatment response to Cognitive-Behavioural Therapy for Insomnia (CBT-I) in psychosis. Schizophrenia research, 221, 57-62. Retrieved from https://doi.org/10.4137%2FSART.S18446, https://journals.sagepub.com/doi/full/10.4137/SART.S18446, and https://www.researchgate.net/profile/Milan-Dragovic/publication/340750291_Different_patterns_of_treatment_response_to_Cognitive-Behavioural_Therapy_for_Insomnia_CBT-I_in_psychosis/links/5ea7ca5fa6fdccd7945b6a83/Different-patterns-of-treatment-response-to-Cognitive-Behavioural-Therapy-for-Insomnia-CBT-I-in-psychosis.pdf.


This was a very interesting read and very helpful! I have been suffering from insomnia since I was a kid and no matter what, sometimes it’s impossible to fall asleep. I never thought about using CBT I, so this article was very helpful. As you said at the end, the paradoxical intention sounds something to try. I always tried to force myself to sleep and has always been counteractive!
I hope it helps
Great post! I’m going to pass this on to my partner as he really struggles with insomnia 🙂 thanks for sharing these benefits x
I hope it helps him
Very interesting read! My sleep has changed lately and I find that I cannot fall asleep as easily! May have to try some of these techniques! Thanks for sharing.
I hope it helps, although you may have to go to a CBT-I therapist to get the full effects from the techniques
I will take these on board as my sleep pattern is crazy sometimes.
Hope it helps
Very informative. I can tell you did a lot of research. Thanks for all the tips. I plan to use some.
Thanks
This CBT-I technique sounds good. Maybe I should try it. I’m also having problem falling asleep sometimes. But I’m not depressed. I’m just too excited with my creative works.
You don’t have to be depressed to use CBT-I
I’ve never heard of CBT for insomnia. Thanks for sharing. ?
Thanka for reading
I’ve has chronic insomnia for about two years and have only recently been able to find ways to manage it that work for me but CBT-I sounds like a great option for if/when my sleep health takes a sh*t again. Would it be okay if I included a link to this post on my post called ‘Supporting Your Mental Health: How To Get Better Sleep’ — I think this is really useful information?
Thanks for asking, and yes you can included a link in your post to link to this one
That’s awesome it helps with insomnia as I know some people who struggle with that. Thank you for sharing!
Thanks for reading
I’ve never heard of CBT-I until now. I’m glad this exists for those who suffer with insomnia. It’s helpful that it discusses the root causes of your insomnia and possible treatment. Thanks for sharing!
Thank for reading
This is such a interesting post. Since falling ill, I suffer with insomnia so I’m defo going to be taking this into consideration! Thank you so much for sharing Xo
Elle – ellegracedeveson.com
I hope the information proves useful
My husband has trouble sleeping a lot of the time and this sounds like it might be a good thing for him to look into! I will definitely pass your article along! Thanks for giving such an in-depth explanation as I have never heard of this before. Most people just recommend medications – which doesn’t seem to work out so well for my husband!
Medications aren’t a long term solution
I have never heard of this type of sleep therapy to help reduce insomnia, but many of the tips you share for creating an inviting sleeping environment, minimizing distractions, and settling into the ‘end-of-day’ mindset are things I often encounter in articles on how to get better sleep, so I love that there is a little cross-over!
Thank you for sharing. <3
I just wish we all lived in environments where they can be optimised for sleep
Wow how scary is the link between insomnia and cancer? As I was reading this, all I could think of was how my poor gran used to suffer from it too. Then it dawned on me. What did she did of??? Cancer! That hot me like a ton of bricks! Thankfully, I don’t take after her in that department. I love sleep and actually look forward in going to bed, and I could sleep through an earthquake. Great read! Thanks for sharing.
When I’m at home and once I fall asleep, nothing wakes me up. I can’t sleep anywhere else, so on holidays or overnight stays somewhere else, I rarely get more than a couple of hours sleep
Thanks for sharing such an insightful post. I always thought that drinking alcohol is a natural sedative and can help with one with Insomnia and reach deep sleep ?.
A lot of people have that belief
This is such an informative post. I never knew insomnia and cancer were so related. I know a friend that has insomnia and it gets terrible sometimes. I would be more than happy to share this post with her. Thank you for sharing.
I hope your friend finds it useful
PTSD plays a huge factor with my insomnia. I’ve never heard of CBT-I before so thanks for sharing this. I’m going to read up more about it and check out the apps too.
I hope you discover something that’ll help you
This is great information. So many sleepless nights over here! Thanks for sharing, I need to do some research about it.
Olivia | https://www.oliviaandbeauty.com
I hope it helps
Great information!
Thanks
I had not heard about CBT before. Its true that sleeping pills help but they are not a long term solution. I used to take Chamomile tea to help me sleep and since I started going to therapy it helped me realize what was causing me to have sleeping troubles. I’m glad that CBT exist and helping people with insomnia.
CBT can be very versatile
This was really informative and helpful. I suffer from insomnia from time to time but it is usually during stressful periods of my life. Thank you for sharing this post!
Stress can really do a number on us
I’ll have to get my husband to try this; he hasn’t been sleeping well and melatonin alone hasn’t helped. I’ve never even heard of CBT…
Melatonin didn’t work for me either, it just gave me heart palpitations. The evidence CBT-I looks really good, so it might be worth while trying one of the CBT-I apps
I find that a change in environment help me a lot. I hardly struggle with sleep issues anymore.
It’s great when you can find something that works